POTS and Lyme disease
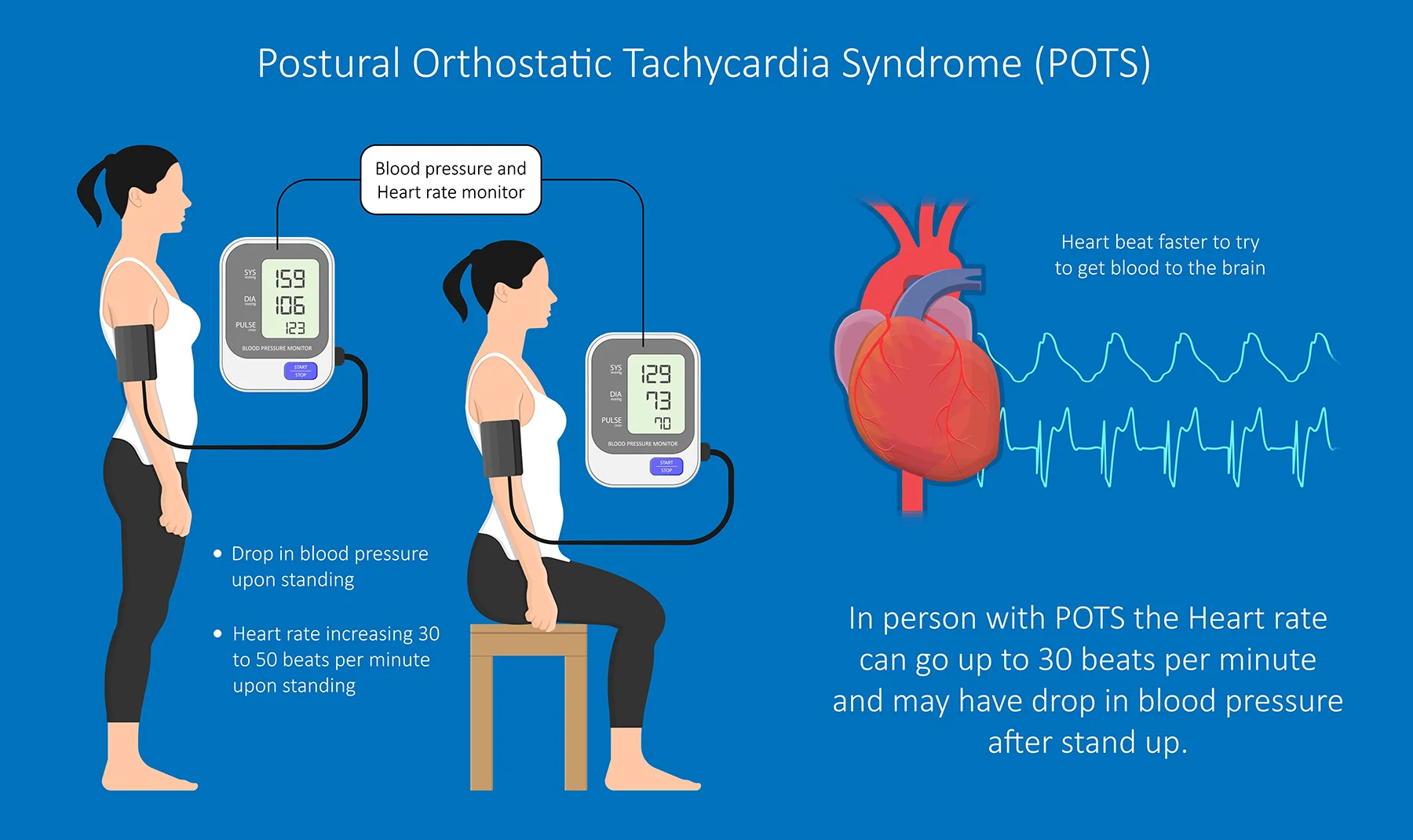
Postural orthostatic tachycardia syndrome (POTS) is a disorder that affects circulation and the body’s ability to regulate blood flow when changing positions. It involves dysfunction of the autonomic nervous system, which automatically controls essential processes such as heart rate, blood vessel constriction, and the body’s “fight or flight” response. A defining feature of POTS is orthostatic intolerance, meaning symptoms become worse when a person moves from lying or sitting to a standing position. Common symptoms include light-headedness, dizziness, fainting, fatigue, and a rapid increase in heart rate upon standing.
Under normal circumstances, heart rate and blood pressure work together to maintain stable blood flow regardless of posture. In people with POTS, however, the coordination between heart rate response and blood vessel constriction becomes impaired, making it difficult to maintain consistent circulation and stable blood pressure when upright. Because POTS involves abnormalities in vascular regulation, circulation, and autonomic nervous system signaling, researchers studying supportive wellness technologies such as pulsed electromagnetic field (PEMF) therapy have shown interest in how electromagnetic stimulation may interact with physiological processes related to circulation and cellular signaling. Readers interested in exploring this area further can review clinical-grade PEMF therapy machines and full-body PEMF systems used in wellness and professional environments.
Every POTS case is unique. Over the course of years, symptoms may come and go for people with POTS. In most situations, a person with POTS will experience an improvement in quality of life with changes to diet, medications, and physical activity. Additionally, if an underlying reason is identified and treated, POTS symptoms may improve.
POTS can take different forms:
- Neuropathic POTS: Loss of peripheral nerve supply causes weak blood vessel muscles, particularly in the legs and core of the body
- POTS with hyperadrenergic symptoms: excessive sympathetic nervous system activation
- POTS can be caused by low blood volume. Similar symptoms that may coexist with neuropathic and hyperadrenergic POTS can be caused by low blood volume.
What does POTS have to do with Lyme disease?
A tick bite can cause Lyme disease. It is a disease that affects various organ systems, such as the heart, muscles, and nerves. Erythema migrans, a rash that appears after a tick bite, is where it starts. Antibiotics typically work to treat Lyme disease, but some people have what is known as the post-Lyme disease syndrome. "Brain fog" is a syndrome of exhaustion, discomfort, and mental haziness that has a negative effect on a person's quality of life. By examining patients with POTS who also had Lyme disease and the post-Lyme disease syndrome, a team of US researchers from Ohio revealed a connection between the two conditions.
Studies on POTS and Lyme disease
A study on the relationship between Lyme disease and POTS syndrome
Five individuals with Lyme disease who had developed fatigue, orthostatic intolerance, and cognitive dysfunction were included in the study. Some people experienced dizziness and fainting, as well as other symptoms like palpitations, poor exercise tolerance, headaches, and mental fogginess. All the patients were so weak that they were confined to their homes. To make a diagnosis of POTS syndrome, tests like tilt table testing and a clinical examination were used.
Patients were treated according to established guidelines by the team, which has extensive experience caring for people with POTS disease. Exercise and increasing sodium and water consumption were advised. If POTS symptoms persisted, medication was administered, with each patient receiving different mixtures of drugs based on what was deemed necessary. If there was an improvement in symptoms, treatments were deemed successful.
The POTS syndrome was successfully treated in all patients. Orthostatic symptoms, particularly weariness, improved in all patients. The passing-out episodes completely disappeared in three patients, whereas they appeared substantially less frequently in the other two. Four out of the five patients were able to get back to their regular daily routines.
The importance of treating POTS syndrome has been proven
This was demonstrated in this study, which included patients with Lyme disease. The post-Lyme disease syndrome, a syndrome that can manifest, has POTS syndrome as a clear characteristic. It was crucial for this group to recognize POTS syndrome because, once treated properly, it led to a reduction in debilitating symptoms and an improvement in quality of life. Therefore, when treating patients with post-Lyme disease syndrome, doctors should have a high degree of suspicion for POTS syndrome. The number of people affected by post-Lyme disease syndrome is unknown in this study; it might be a small percentage. However, it was crucially shown that a focused and organized approach to treatment can greatly increase the quality of life for those with POTS.
How does POTS present?
POTS can start gradually or unexpectedly for some people. Occasionally, you may have symptoms right away or a few minutes after standing or sitting up. The severity of some symptoms could be reduced by lying down.
The following are typical POTS symptoms:
- feeling unsteady or light-headed
- heart palpitations, fainting, problems with thinking, memory, and concentration—this combination of symptoms is frequently referred to as "brain fog"
- trembling and perspiration, weakness, and exhaustion (tiredness)
- headaches
- difficulty sleeping
- chest discomfort
- nausea
- breathlessness
- Some people discover that getting heated, eating, engaging in vigorous exercise, or going through their period can exacerbate their symptoms.
When to consult a doctor
Consult a qualified healthcare professional if you suspect you may have postural orthostatic tachycardia syndrome (POTS). Obtaining an accurate diagnosis is important because the symptoms can overlap with several other conditions, including low blood pressure, autonomic disorders, or medication-related effects. In some cases, POTS symptoms may even be mistaken for anxiety or panic episodes. A proper medical evaluation can help identify the underlying cause of symptoms and guide appropriate management strategies.
Diagnosis of POTS
When your heart rate increases by at least 30 beats per minute (bpm) and typically within 10 minutes of standing (40 bpm in children and adolescents aged 12-19 years), POTS is suspected. With this increase in the heart rate, other POTS symptoms may occur that last longer than 30 seconds.
To confirm a diagnosis and rule out other diseases, you might undergo various tests, such as:
- The tilt table test involves lying on a special bed that can be tilted upright while your blood pressure and heart rate are monitored. More measurements are taken when the bed is gradually tilted towards a more upright position.
- Active stand test: when you stand up from lying down, your heart rate and blood pressure are recorded. They are then recorded after 2, 5, and 10 minutes.
- An echocardiogram, which is an ultrasound scan of your heart, and an electrocardiogram (ECG), which measures the electrical activity of your heart
- Holter monitoring: small, belt-mounted gadgets that continuously measure your pulse rate and blood pressure while you perform your daily business
- Blood tests are used to check the health of your kidneys, liver, and thyroid, as well as your blood count, calcium levels, and glucose levels.
Treatment of a POTS Occurence
Self-care strategies can sometimes help reduce symptoms of postural orthostatic tachycardia syndrome (POTS), although some individuals may still require medication if symptoms persist. When feelings of light-headedness or faintness occur, improving blood flow to the brain may help reduce symptoms. Lying down and elevating the legs, when possible, can encourage circulation back toward the upper body. If lying down is not possible, certain physical counter-maneuvers may help temporarily support circulation while standing. These can include gently rocking or swaying on the toes, crossing the legs while standing, tightening the muscles of the abdomen and buttocks, or clenching the fists to help promote blood flow and stabilize blood pressure.
Medications and Wellness Options for POTS:
There is no single medication that treats postural orthostatic tachycardia syndrome (POTS), and treatment approaches often vary depending on the individual and the underlying causes of symptoms. Physicians may recommend medications that help manage heart rate, blood vessel tone, or fluid balance, including:
- Beta blockers or the heart-rate–lowering drug ivabradine to help control tachycardia
- Midodrine to promote blood vessel constriction and support blood pressure when standing
- Fludrocortisone to reduce sodium loss during urination and help maintain blood volume
- Selective serotonin reuptake inhibitors (SSRIs), a class of antidepressants that can influence autonomic nervous system signaling
Because POTS involves complex interactions between circulation, autonomic regulation, and vascular responsiveness, researchers studying supportive wellness technologies have also explored whether modalities such as pulsed electromagnetic field (PEMF) therapy may interact with physiological processes related to circulation and nervous system signaling. Readers interested in learning more about PEMF technology can review clinical-grade PEMF therapy machines and full-body PEMF systems used in wellness and professional environments.
RELATED POSTS